- ANFP TV
- Edge: Fuel Your Filter: Nutrition Therapy for Liver Healthy
Edge: Fuel Your Filter: Nutrition Therapy for Liver Healthy
By Kathy Murdock, MS, RD, LD
September 29, 2025
This Nutrition Connection CE article appeared in the September/October 2025 issue of Nutrition & Foodservice Edge magazine. To view a PDF of this article click HERE.
To earn 1.0 GEN CE credit, purchase the CE article in the ANFP Marketplace HERE or click the button below and complete the quiz.
This course is a level II continuing competence. View continuing competence level descriptions HERE.

Fuel Your Filter: Nutrition Therapy for Liver Healthy
By: Kathy Murdock, MS, RD, LD
The pain comes and goes, so Frankie just assumed it was her gallbladder. When she saw the doctor, the ultrasound indicated she had mild fatty liver. Frankie’s labs came back normal with the exception of triglycerides, which were only slightly elevated, and her cholesterol was “borderline” per the nurse. She was told to follow a healthy diet and to exercise. Frankie’s weight was 155 and her height 64” with a BMI of 26.6, indicating she was overweight. She rarely eats out and only drinks alcohol occasionally (less than two drinks a month). To help with the pain and in an attempt to correct triglycerides and cholesterol, Frankie started an exercise routine and adopted a diet similar to the Mediterranean diet. After losing 10 pounds and two months of following the diet on most days, the pain in her right upper abdomen resolved. Surprisingly, she also realized her brain fog and fatigue improved. When she returned for a check-up, her triglycerides and cholesterol levels were within normal ranges.
LIVER HEALTH OFTEN TAKES A BACK SEAT when discussing nutrition for prevention and treatment of chronic diseases. However, the liver is a powerhouse and performs vital functions such as detoxification, nutrient metabolism, and hormone regulation. The accumulation of fatty tissue in the liver can disrupt these functions. The prevalence of non-alcoholic fatty liver disease (NAFLD) has risen to over 30 percent of the population. NAFLD can be linked to poor diet and a sedentary lifestyle. There are no medications to treat NAFLD, and in addition to exercise, nutrition therapy can help to treat and, in some cases, possibly reverse the condition.
WHAT DOES THE LIVER DO?
The liver is an amazing organ, working to keep our metabolism on track and our bodies in tip-top shape. It acts as a filter for the body, removing toxins and metabolizing drugs, alcohol, and excess fat. It produces bile, a fluid that emulsifies fat and aids in its digestion and waste elimination. It regulates glucose by converting excess sugar into glycogen for storage and releasing it when needed. The liver is vital to protein metabolism, converting wastes like ammonia into urea for excretion. It also stores iron and fat-soluble vitamins (A, D, E, K), along with the water-soluble vitamin B12, and metabolizes hormones such as insulin and estrogen. When liver function is impaired —as in NAFLD—these processes are disrupted, leading to an accumulation of toxins, impaired nutrient metabolism, and inflammation. The results can significantly impact the body’s overall well-being.
SYMPTOMS AND CONSEQUENCES OF NAFLD
In the initial stages of NAFLD there are often no obvious symptoms or they are mild and can be overlooked. These symptoms may include:
- Fatigue
- Discomfort or pain in the upper right abdomen
- Elevated liver enzymes on blood tests
- Insulin resistance and metabolic syndrome
- Nutrient deficiencies
Micronutrient Deficiencies in NAFLD
Individuals with NAFLD may have low levels of several important micronutrients. Because the liver is vital in micronutrient absorption, many other symptoms may occur when these micronutrients become deficient. The following are several vitamins and minerals of concern:
- Vitamin D – Associated with inflammation and insulin resistance; deficiency is common in advanced liver disease.
- Vitamin E – Acts as an antioxidant; low levels can cause increased oxidative stress and liver damage.
- Vitamin A – Stored in the liver; deficiency can impair immunity and increase injury to the liver.
- B-complex Vitamins – Particularly folate (B9) and B12, which are important for methylation, DNA repair, and reducing homocysteine levels.
- Zinc – Helps in liver repair and antioxidant defense.
- Selenium – A cofactor for glutathione peroxidase; deficiency disrupts oxidative balance.
- Choline – Helps to remove fat from the liver; deficiency can contribute to steatosis.
DOES DIET MAKE A DIFFERENCE?
Diet plays a significant role in both the development and management of NAFLD. Excessive consumption of saturated fats, added sugars, and ultra-processed foods has been directly linked to fat accumulation in the liver. A whole-food diet rich in antioxidants, fiber, and healthy fats can improve liver function and may reverse early NAFLD. The Mediterranean diet is one of the diets often prescribed for individuals diagnosed with fatty liver, due to its high fiber content, nutrient density, and is low in saturated fats.
Foods to Reduce
There is extensive research on the effects of certain foods on liver health. The Western diet is often high in the following, which can contribute to the development of many chronic conditions, including NAFLD:
- Ultra-processed foods (chips, sweets/desserts/pastries, frozen meals)
- Sugar-sweetened beverages, fructose-heavy sweeteners, especially high-fructose corn syrup
- Refined carbohydrates (white bread, pasta, pastries)
- Saturated and trans fats (fried foods, processed meats)
- Excessive alcohol: even though NAFLD is non-alcoholic, consumption of alcohol can cause further damage to the liver
These foods contribute to inflammation, insulin resistance, and excessive caloric intakes, which can lead to fat accumulation in the liver.
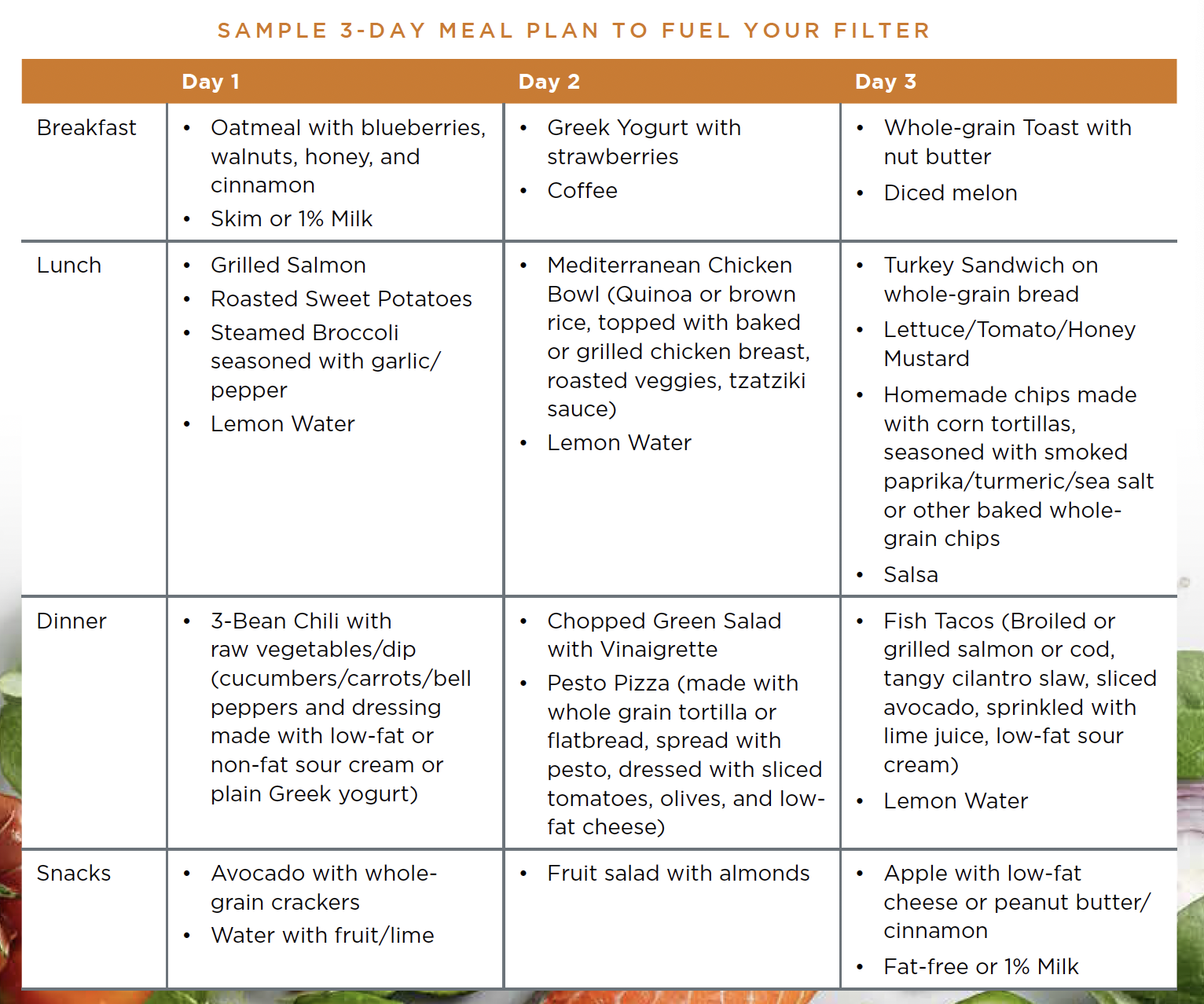
Foods to Include
For optimal liver health, a whole foods diet limiting ultra-processed foods, refined carbohydrates and saturated fats, should include the following:
- Fruits and vegetables – Rich in antioxidants (vitamins A, C, E) and polyphenols to reduce oxidative stress
- Whole grains and legumes – Provide fiber for glycemic control and satiety
- Lean proteins – Support
- muscle mass and liver enzyme production
- Fatty fish (e.g., salmon) – High in omega-3 fatty acids, which reduce liver fat and inflammation
- Nuts and seeds – Provide healthy fats, zinc, and selenium
- Coffee (in moderation) – Associated with reduced liver fibrosis and lower ALT (alanine transaminase) levels
These foods offer anti-inflammatory and antioxidant benefits, improve insulin sensitivity, and help reduce fat accumulation in the liver. Following these recommendations can lead to reduced calorie consumption and support healthy weight loss.
OTHER CONSIDERATIONS
Along with specific diet changes, the following can also benefit liver health:
- Weight loss of 7–10 percent has been found to reduce liver fat and inflammation.
- Intermittent fasting, according to Lange, et al., may help to improve liver function and aid in weight loss.
- Physical activity, especially resistance and aerobic exercise, enhances insulin sensitivity in the liver.
- Regular screening of liver function and nutrient levels in patients at risk (e.g., those with obesity or diabetes).
CONCLUSION
The liver is vital to many aspects of metabolic health. Medical nutrition therapy offers a powerful and practical strategy for the prevention and treatment of NAFLD. As with Frankie, changing the diet can have a significant impact on the effects of fatty liver. By reducing harmful foods and emphasizing nutrient-dense, anti-inflammatory dietary patterns, individuals can improve liver function and overall health to fuel the body’s most important filter.
About the Author
Kathy Murdock, MS, RD, LD
Kathy Murdock has been working in nutrition and dietetics since 2007. She is currently a consultant dietitian in long-term and acute care in rural southeast Missouri and northeast Arkansas. She has a passion for teaching, writing, and public speaking. Murdock previously worked for a community college in northeast Arkansas teaching future CDM, CFPPs.









