- ANFP TV
- Edge Express: Crafting Meals with Culture & History
Edge Express: Crafting Meals with Culture & History
By Kristin Klinefelter, MS, RDN, LDN
June 11, 2025
This Nutrition Connection CE article appeared in the June 2025 issue of Nutrition & Foodservice Edge Express. To view a PDF of this article click HERE.
To earn 1.0 GEN CE credit, purchase the CE article in the ANFP Marketplace HERE or click the button below and complete the quiz.
This course is a level III continuing competence. View continuing competence level descriptions HERE.

Crafting Meals with Culture and History: How Nostalgia Can Transform Nutrition and Enhance Intake
By: Kristin Klinefelter, MS, RDN, LDN
A CORE MEMORY I ASSOCIATE WITH FOOD is the last day I spent with my Grandma Ellen. A strong-willed woman of 100 percent Norwegian heritage, she expressed love through cooking. When I asked her to teach me how to make lefse, she immediately agreed. We spent the next day in the kitchen, laughing over my clumsy technique. It was the last day we were together. That lefse recipe now lives on through my daughters and me, connecting us to Grandma Ellen’s memory, culture, and love.
Food is not just sustenance; it’s a sensory gateway to memory, identity, and dignity. The limbic system, which regulates emotion and long-term memory, is closely tied to smell and taste. Herz and Schooler (2002) demonstrated that odor-evoked memories are more emotional than memories triggered by sight or sound. For older adults, especially those in long-term care, these memories are powerful therapeutic tools.
Nostalgia is increasingly recognized in geriatric nutrition and dementia care as a compelling tool for emotional and therapeutic engagement. Culturally and religiously significant meals — especially those tied to holidays, family traditions, and life milestones — can support identity, foster belonging, and enhance overall well-being. For a Certified Dietary Manager, Certified Food Protection Professional (CDM, CFPP), these meals present opportunities to deliver meaningful, person-centered experiences that go beyond basic nutrition.
Among the most potent memory triggers are smell and taste. This is the basis of the Proust Effect, a term inspired by Marcel Proust’s In Search of Lost Time, where the taste of a madeleine dipped in tea evokes a vivid flood of childhood memories.
Scientific research supports this phenomenon. De Bruijn and Bender (2018) found that olfactory cues were significantly more effective than visual stimuli in evoking detailed and emotionally rich autobiographical memories. Similarly, Herz and Schooler (2002) demonstrated that scent-induced memories are more emotionally charged and more closely tied to personal identity than those triggered by sight or sound.
This effect is especially relevant in dementia care. El Haj et al. (2018) found that individuals with Alzheimer’s disease could spontaneously recall long-term memories when exposed to familiar scents. These odor-evoked memories were emotionally significant and involuntary, offering therapeutic potential to stimulate cognition and improve quality of life.
In a broader context, Herz (2016) emphasized that scent-triggered memories promote both psychological and physiological well-being by enhancing mood, reducing stress, and fostering a sense of safety. For CDM, CFPPs, this underscores the value of integrating aroma-rich, culturally familiar dishes into therapeutic menus. Whether it’s the smell of freshly baked challah, simmering soup, or dill-scented potatoes, these aromas provide a sensory bridge to cherished memories, supporting emotional connection, dignity, and quality of life in nutrition care.
A familiar scent or flavor can transport individuals directly back to the memory itself. The smell of fresh bread, old books, or a delicious bowl of soup can bring up powerful feelings of love, safety, and personal history. For residents in long-term care, particularly those with cognitive decline, these moments of reconnection can feel like a warm embrace from their past.
For CDM, CFPPs, recognizing and leveraging this phenomenon means creating intentional, individualized dining experiences. We should consider not just therapeutic dietary modifications, but the personal and cultural stories clients carry with them. Meals infused with familiar scents and flavors can transform nutrition from a routine into a moment of dignity, healing, and joy.
The reason smells trigger such vivid emotions and memories lies in the unique way the brain processes information triggered by the sense of smell. Unlike other senses, such as vision or hearing, which first pass through the brain’s thalamus (the brain’s relay center), the sense of smell bypasses this structure entirely. When odor molecules enter the nose, they bind to specialized olfactory receptors located in the nasal cavity. These receptors generate electrical signals that travel directly to the olfactory bulb, the brain’s processing hub for smell.
From there, the signal takes a direct route to two regions of the limbic system: the hippocampus, which plays a role in long-term memory formation, and the amygdala, which governs emotional processing (also the “fight, flight or freeze” center for stress response). This “shortcut” explains why certain scents can evoke deeply personal, emotional, and often involuntary memories almost instantaneously.
From an evolutionary standpoint, this mechanism likely served as a critical survival function. Early humans used their sense of smell to detect environmental threats, locate food, and identify familiar people or places. As a result, olfactory processing became tightly linked with memory and emotion, ensuring that important experiences, especially those involving safety or danger, would be quickly and vividly remembered.
Today, this powerful neural connection allows a simple scent like cinnamon, fresh grass, or baked bread, to transport someone back decades in a single sniff.
CDM, CFPPs act as the “voice of the plate,” ensuring meals are not only safe and nutritious but emotionally significant. Their role includes honoring residents’ culinary histories while upholding individualized clinical nutrition interventions.
CLINICAL CONDITIONS AND CULTURAL ADAPTATIONS
Diabetes
Older adults with diabetes must control carbohydrates while maintaining adequate intake of protein, magnesium, calcium, and other key nutrients. CDM, CFPPs can adapt cultural meals in various ways.
- Swap white rice for lower glycemic grains like quinoa or barley.
- Use sweeteners like stevia for traditional desserts.
- Offer smaller portions of starch-rich cultural favorites.
Example: For a Jewish client during Hanukkah, a CDM, CFPP could prepare baked latkes using grated zucchini and sweet potatoes, paired with unsweetened applesauce.
Chronic Kidney Disease (CKD)
Residents with renal failure need to limit phosphorus, sodium, and potassium while consuming individualized protein levels.
- Replace tomato sauces with roasted red pepper purée.
- Use herbs instead of salt to maintain flavor.
- Choose low-potassium alternatives like apples or green beans over bananas or potatoes.
Example: A Scandinavian-inspired cod dish with mashed cauliflower and dill provides a nostalgic flavor while remaining renal-friendly.
Dysphagia
CDM, CFPPs trained in the International Dysphagia Diet Standardisation Initiative (IDDSI) framework can recreate cultural textures and shapes using molds and garnishes to make meals recognizable and appealing.
Example: A pureed version of Southern fried chicken shaped into a cutlet, served with smooth sweet potato mash and gravy, offers dignity and enjoyment through visual and taste cues.
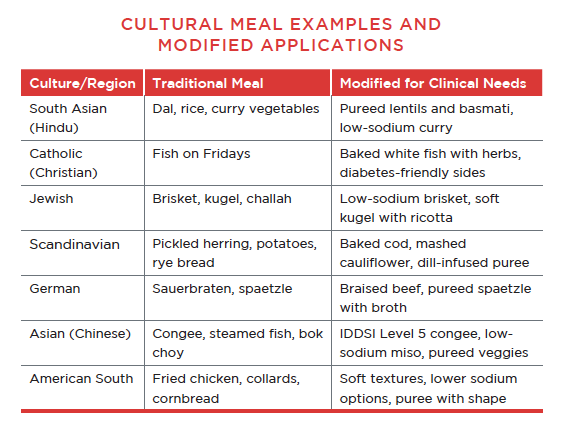
CREATING MEANINGFUL EXPERIENCES, EVEN ON THERAPEUTIC DIETS
CDM, CFPPs can help infuse joy and comfort into clinical nutrition if they:
Host Cultural Theme Days
- Example: “Italian Heritage Day,” featuring tomato-free pasta sauces for CKD clients and almond flour biscotti for diabetics.
- Include visuals, music, and table décor to engage all senses.
Offer Memory Trays
- Small nostalgic tasting plates (e.g., German spaetzle or Scandinavian lingonberries) tailored to therapeutic needs.
- Ideal for clients with memory loss or low appetite.
Present Intergenerational Programs
- Invite children to learn about lefse, matzo, or tamales from residents.
- Supports dignity, purpose, and storytelling.
Provide Personalized Recipe Revival
- Work with family members to adapt beloved recipes into therapeutic versions.
- Print “Family Favorites” cookbooks as legacy projects.
CBDM PRACTICE DOMAINS ALIGN WITH GOALS
The Certifying Board for Dietary Managers (CBDM) Practice Domains align with nutrition goals.
- Domain I: Nutrition – CDM, CFPPs reinforce therapeutic diets with culturally appropriate substitutions.
- Domain II: Foodservice Systems – CDM, CFPPs oversee kitchen staff in preparing safe, modified meals.
- Domain III: Personnel and Communication – CDM, CFPPs coordinate with RDNs, families, and care teams.
- Domain IV: Sanitation and Safety – CDM, CFPPs ensure safe handling of traditional ingredients.
- Domain V: Business Operations – CDM, CFPPs use seasonal or bulk cultural ingredients cost-effectively.
SUMMING IT UP
Food memories can unlock joy, identity, and appetite, especially in clinical settings where clients may have dietary or mobility restrictions. CDM, CFPPs, grounded in both foodservice expertise and cultural empathy, are uniquely positioned to lead this transformation. Through person-centered, nostalgia-enhanced meals, they nourish not just bodies, but hearts and histories.
About the Author
Kristin Klinefelter, MS, RDN, LDN
Kristin Klinefelter has been trying to make her Grandma Ellen proud with her sub-par lefse making skills for decades. She was even quoted in the book: The Last Word on Lefse, by Gary Legwold. When not making lefse, Klinefelter is an instructor with UND’s Nutrition & Foodservice Professional Training Program, teaches at local community colleges, writes, speaks, and consults in foodservice and business operations.









