- ANFP TV
- Edge: The Power of Protein: Benefits and Menu Considerations
Edge: The Power of Protein: Benefits and Menu Considerations
By Chrissy Carroll, MPH, RD
July 17, 2024
This Nutrition Connection CE article appeared in the 2024 July/August issue of Nutrition & Foodservice Edge magazine. To view a PDF of this article click HERE.
To earn 1.0 GEN CE credit, purchase the CE article in the ANFP Marketplace HERE or click the button below and complete the quiz.
ANFP members may save 20% on this article through July 9, 2025, thanks to our sponsor:

This course is a level II continuing competence. View continuing competence level descriptions HERE.

The Power of Protein: Benefits and Menu Considerations
By: Chrissy Carroll, MPH, RD
PROTEIN IS A POWERHOUSE NUTRIENT for any population, but especially for older adults and school-age children. Understanding the benefits of protein, being knowledgeable about daily requirements, and creating innovative menu solutions can help you improve the health and well-being of those you serve.
PROTEIN AND OLDER ADULTS
Adequate protein intake is one of the most important nutrition considerations for older adults. Getting enough protein (and calories) can reduce the risk of malnutrition, a major concern in hospitals and long-term care facilities. Recent research suggests anywhere from 8 to 50 percent of patients arrive at long-term care or hospital settings already malnourished, and malnutrition rates often increase after admission. Protein provides essential calories and amino acids to reduce the risk of malnutrition and maintain body weight.
Protein is also key for preserving muscle mass. Sarcopenia, age-related loss of muscle mass and strength, is a common issue among older adults. Preventing sarcopenia is essential for maintaining mobility and decreasing the risk of falls. Protein provides amino acids, which are the building blocks of muscle. There is evidence that frail older adults and those with diagnosed sarcopenia consume less protein than their healthy counterparts.
Lastly, protein is vital for the repair and regeneration of tissue during wound healing. Protein is necessary to develop new blood vessels, produce collagen, and create tissue in the wounded area. Older adults with a wound that have inadequate protein intake may suffer from increased infection risk and slower rates of wound closure.
The Recommended Dietary Allowance (RDA) for older adults is 0.8 grams of protein per kilogram of body weight per day, but needs can vary based on weight, physical activity, and medical conditions. In addition, research suggests that optimal protein intake for healthy older adults may be considerably higher than the RDA. A meta-analysis in Ageing research reviews found that eating higher levels of protein was linked to better physical exercise performance and greater muscle strength in older adults.
Many experts suggest that older adults aim for at least 1.0 to 1.2 grams of protein per kilogram of body weight per day. During times of wound healing, those needs increase to 1.2 to 1.5 grams of protein per kilogram of body weight per day.
Research shows some older adults aren’t even meeting the baseline RDA, though, let alone potentially higher requirements. In fact, studies show anywhere from 5 percent to 46 percent of older adults don’t meet requirements for protein intake. In addition, a 2021 study in Clinical Nutrition found that protein intake often declines over time among long-term care residents. As such, ensuring residents get enough protein is incredibly important throughout their time in the facility.
PROTEIN AND CHILDREN
Protein is equally important for children, who are in stages of rapid growth and development. Protein supplies amino acids that are necessary for building and maintaining healthy muscles, skin, hair, nails, and blood. Getting enough protein may also play a role in regulating healthy body composition among children.
Children aged 4-13 require approximately 0.95 grams of protein per kilogram of bodyweight per day, with teens age 14-18 requiring around 0.85 grams per kilogram per day. However, research from 2021 in Nutrients notes that active children may have needs closer to 1.1 to 1.55 grams per kilogram.
Luckily, most children have no problem meeting their protein needs. However, children who are picky eaters, children with allergies, or children with conditions like Avoidant/Restrictive Food Intake Disorder (ARFID) may have a tougher time meeting guidelines.
PROTEIN CONSIDERATIONS FOR YOUR MENU
Foodservice managers should strive to include a variety of protein sources on the menu. Exact amounts vary depending on the requirements of the population you serve (like the guidelines described previously) and any requirements for your meal program. For example, schools participating in the National School Lunch Program must serve a particular number of meat/meat alternative ounce equivalents along with milk as part of daily meals, both of which contribute to a child’s protein needs.
Aside from specific amounts, there are other factors to consider when planning protein choices for your menu:
Animal vs. Plant-Based Sources
Both types of protein can be included in a balanced diet. Animal sources of protein generally contain all the essential amino acids (the amino acids our bodies can’t make and need to obtain from food), making them a complete protein. Most plant-based protein sources are incomplete, meaning they fall short in one or more essential amino acids.
However, serving a wide variety of plant-based proteins throughout the day can provide a complete amino acid profile. Incorporate proteins from different categories like grains, legumes, and nuts and seeds. For example, a vegan menu might serve whole grain toast with peanut butter as part of breakfast; a lentil, vegetable, and brown rice soup at lunch; trail mix for a snack; and black bean tacos for dinner. Focusing on variety helps ensure that you’re providing all essential amino acids.
Keep in mind that animal proteins generally provide the largest amount of protein in the smallest volume of food. Because of this, animal protein sources are often helpful in older adults with reduced appetite. Eating a small portion can provide them with quite a bit of protein. For example, serving 3 ounces of lean sirloin steak—about the size of a deck of cards—provides about 26 grams of protein. Someone would have to eat around 1 ½ cups of black beans with 1 cup of brown rice to reach the same amount of protein. The volume can be problematic if appetite is low.
Overall, consider the preferences and needs of your audience when choosing protein sources for your menu. You’ll likely want to include a variety of both options. You can see sample animal and plant sources with their protein content in the sidebar.
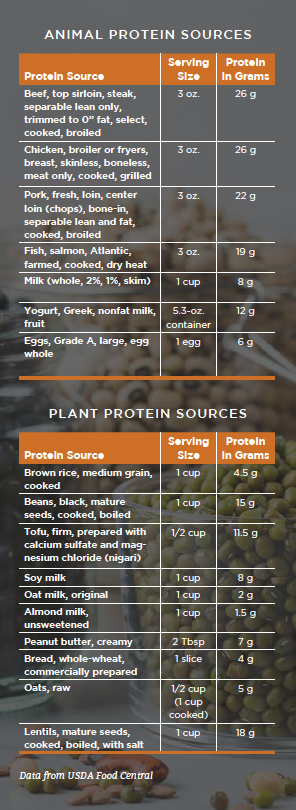
Nutrient Density
Many sources of protein also provide additional nutrients, and these vary based on the type of food. For example:
- Dairy products provide calcium and Vitamin D, essential for bone health.
- Fatty fish provides omega-3 fatty acids, which are important for brain and heart health.
- Beans supply dietary fiber to support the digestive system.
- Eggs provide choline, linked to cognitive health.
- Oats deliver beta-glucan, a soluble fiber that’s beneficial for cholesterol.
- Nuts contain antioxidants, which can help fight cell damage.
- Lean beef contains minerals like iron and zinc, involved in blood and immune health.
Offering a variety of protein sources (and other food sources in general) throughout the week helps ensure optimal intake of all nutrients.
Allergens
Several common sources of protein, like dairy, nuts, peanuts, fish, and shellfish, fall into the top nine most common food allergens. Diagnosed food allergies have grown tremendously over the last 30 years. In 1997-1999, the prevalence of food allergies among those 0 to 17 years old was 3.4 percent, while in 2021, that increased to 5.8 percent. That represents 70 percent growth!
Offering alternative protein sources can accommodate residents or students with allergies. For example, soy milk could be served rather than dairy milk for an elementary-aged child with a food allergy. Seed butters could be used as a spread rather than peanut butter for an adult with a peanut allergy. Other animal proteins like chicken, turkey, or pork could be substituted for seafood in the case of a fish allergy.
Be sure to check the regulations that exist for your particular foodservice operation, as guidelines on substitutions vary based on the facility and program. Ideally, substitutions should be of similar nutritional value.
Cultural and Religious Preferences
The United States is a rich tapestry of diversity, and foodservice managers will continue to see an increase in demand for foods that honor cultural or religious traditions. It’s important to consider these factors when deciding on the protein choices at your facility.
For example, a school that serves a large Muslim population may eliminate pork from the menu, as it’s traditionally not eaten under religious traditions. A long-term care facility that serves a large Haitian population may wish to include soup joumou on the menu on January 1, a Haitian beef, vegetable, and squash soup served to commemorate Haiti’s liberation from French colonial rule.
Reflect on your specific population’s preferences. Consider surveying your population to help guide menu development. For example, the CDC recommends asking questions like:
- What types of foods are embraced by your culture?
- Do you have any cultural habits or traditions related to foods you like to eat? What about foods you prefer not to eat?
- Do you enjoy eating cultural foods away from home, or do you prefer eating other types of foods away from home?
- What are some barriers to eating your favorite cultural foods in this facility?
- What are some recommendations for improving our food offerings?
- What are your favorite items currently on our menu?
Answers to these questions can help you determine if there are certain types of menu additions or changes that should be considered. Keep in mind that each individual person may have different opinions or preferences, despite being from the same culture or religion as another person.
Protein Timing
Most folks tend to “backload” protein, eating very little at breakfast and the majority at either lunch or dinner (depending on the age group). However, spacing protein intake more evenly throughout the day could better support optimal muscle health and assist in satiation after meals.
In fact, a study in Nutrition Journal found that frail older adults showed a more uneven distribution of protein intake, eating little at breakfast, compared to non-frail participants. Similarly, a study in Frontiers in Nutrition suggests morning protein intake plays an important role in muscle mass and physical function metrics in older adults.
Foodservice managers should aim to have good sources of protein at each mealtime. Breakfast is often the most challenging meal, so here are some higher protein breakfast ideas to consider:
- Breakfast burrito with beans, veggies, salsa, and cheese
- Oatmeal made with milk, egg whites, or protein powder, along with peanut butter and fruit
- Lean beef or turkey breakfast burger with mushrooms, egg, tomato, and arugula
- Waffle breakfast sandwich with eggs, ham, cheese, and greens
- Protein fortified pancakes served with fruit and sunflower seed butter
- Greek yogurt parfait with peanut butter and berries
- Smoothie made with whey or plant-based protein powder
- Savory quinoa with eggs and spinach
- Whole grain toast with ricotta, fruit, nuts, and a drizzle of honey
- Breakfast hash made with ground turkey, peppers, onions, and sweet potatoes
- Salmon patty breakfast sandwich
Fortified Foods and Supplements
If a person cannot meet their protein needs through traditional food sources alone, fortified foods and supplements can be a useful tool, especially in long-term care and hospital settings.
Fortified foods can be made in-house, or you can purchase specific options from vendors. For example, you could add powdered milk to soups, add egg whites when cooking oatmeal, or make dips using blended cottage cheese, all of which can boost protein in the final dish. Similarly, protein powders can be used in baked goods like muffins, pancakes, waffles, and quick breads, as well as in options like smoothies and ice cream. In fact, a 2022 study in the Journal of Texture Studies found that whey protein can be added to thickened ice cream without any impact on the acceptability or enjoyment of ice cream in long-term care residents with dysphagia and wounds. You could also purchase products directly from vendors, like protein-fortified ice cream or pudding.
Using protein-enhanced foods is impactful, as research suggests it can increase protein intake in clinical settings. A study in Geriatrics found that an energy- and protein-enhanced diet (created by fortifying recipes in-house) led to an improvement in nutritional status of older adults.
Oral nutrition supplements are another option, and include a variety of prepared protein drinks like shakes, smoothies, and juices. Typically, it’s best to provide these between meals, rather than during mealtimes. Oral nutrition supplements can benefit older adults who struggle to meet protein needs (especially during wound healing), and may also benefit children with picky eating or ARFID who are struggling with growth due to lack of intake.
THE BOTTOM LINE
Protein is a vital component of a balanced diet, especially among children and older adults. It’s essential to make sure your population is meeting their needs. Implementing a variety of protein options that fit appetite, nutrient needs, allergen concerns, and cultural preferences can ensure that folks maintain their health, recover from illness, and support growth and development.
About the Author
Chrissy Carroll, MPH, RD
Chrissy Carroll is a registered dietitian, freelance writer, and brand consultant based in central Massachusetts.









